AI Radiology Reporting: What the Evidence Says About Accuracy
Reviewed by board-certified radiologists

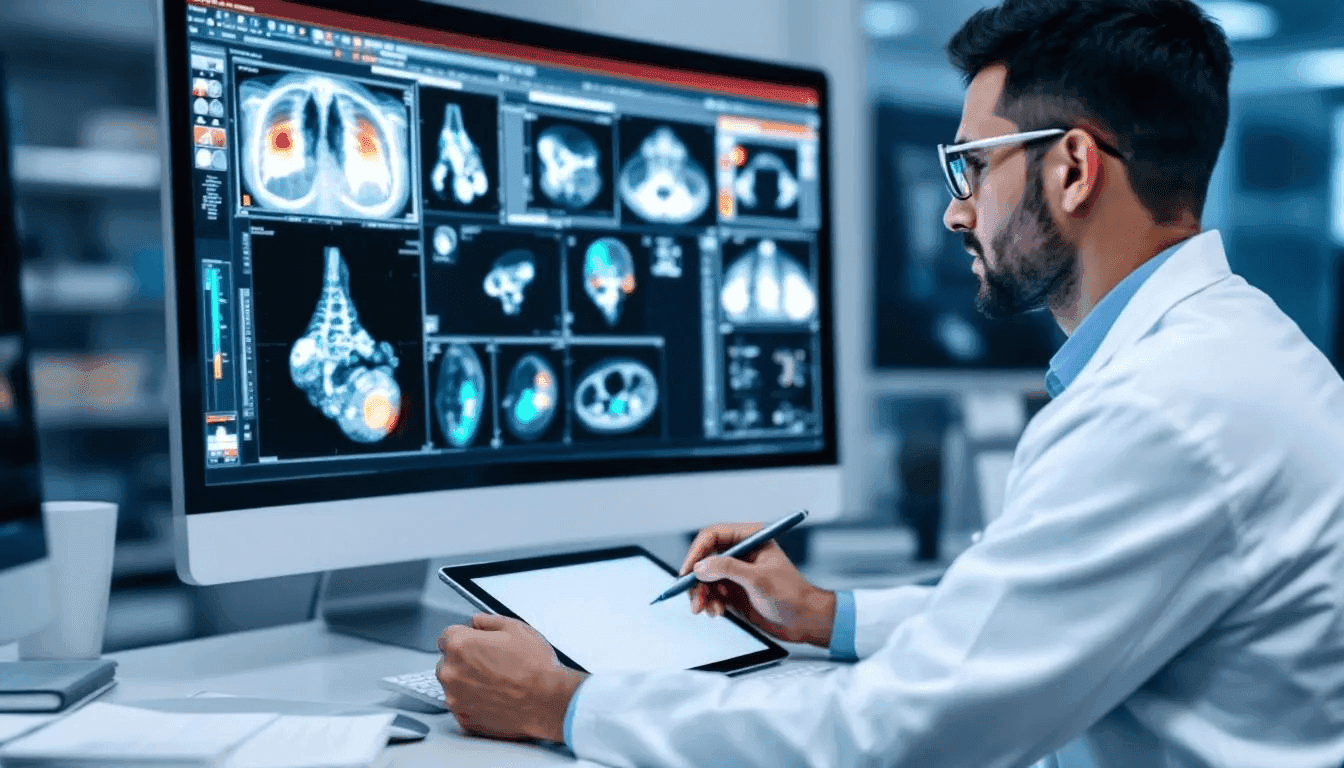
Vendors selling AI radiology tools make bold claims about diagnostic accuracy. "Matches expert radiologist performance." "Detects findings missed by humans." "Reduces false negatives by X%." How much of this is real, and how should imaging centers evaluate AI accuracy claims when choosing a teleradiology partner?
What the Published Evidence Shows
The peer-reviewed literature on AI in radiology is substantial and generally positive, but with important nuance. AI performs well in high-prevalence, pattern-recognition tasks on high-quality images from the training distribution. It performs less well on rare findings, unusual presentations, and images that differ significantly from training data.
- Chest X-ray AI: Multiple FDA-cleared algorithms show sensitivity for pneumothorax, pleural effusion, and pulmonary nodules comparable to experienced radiologists on retrospective test sets. Prospective clinical performance is slightly lower but still clinically meaningful.
- CT pulmonary embolism detection: AI detection of PE on CTPA has reached radiologist-level sensitivity in published studies, with particularly strong performance at reducing time-to-notification for positive cases.
- Diabetic retinopathy and mammography: Two of the strongest AI evidence bases in medical imaging. FDA-cleared algorithms for both have shown sensitivity/specificity comparable to specialist readers in prospective trials.
- General MRI and complex CT: Performance is more variable. AI is a useful assistant for complex MRI interpretation but should not be evaluated as a standalone reader — the human radiologist remains essential.
FDA Clearance vs. Marketing Claims
When evaluating AI in teleradiology, FDA clearance is the minimum bar for clinical use in the US — not just a marketing differentiator. FDA clearance via the 510(k) or De Novo pathway requires the manufacturer to submit clinical evidence that the device performs as labeled. Cleared status means the algorithm has been evaluated against a specific intended use in a clinical population.
Ask any teleradiology provider using AI: which specific algorithms are FDA cleared, for which intended use, and on what study types? Vague references to "AI" without specific clearances are a red flag.
The Right Role for AI in Teleradiology
Natoe AI's position on AI in radiology is clear: AI is a clinical decision support tool that makes board-certified radiologists faster and more consistent — not a replacement for radiologist judgment. Every Natoe AI study is reviewed and signed by a licensed radiologist. AI flags findings, measures structures, and generates report templates. The radiologist interprets, integrates clinical context, and takes clinical accountability. This is the model supported by both the evidence and FDA regulatory framework.